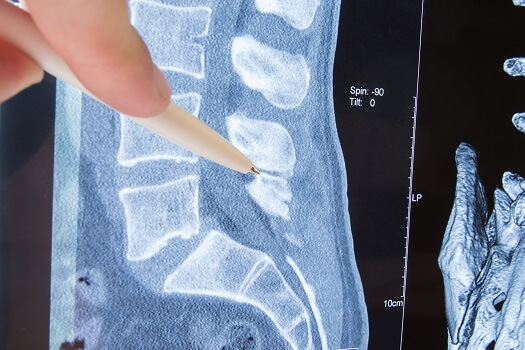
Narrowing of the spinal canal, known as spinal stenosis, tends to progress over time, which is why some people who have had this condition with little or no discomfort for many years sometimes begin to develop disruptive symptoms later in life. If you have spinal stenosis, treatment will depend on what part of the spine is affected and how the narrowing is affecting nearby nerves. However, it’s not a good idea to completely hold off on any type of treatment for spinal stenosis. Here’s why.
Emergency Situations May Occur
A narrow spinal passage sometimes squeezes sensitive nerve roots and the spinal cord itself. With spinal stenosis in the lumbar (lower) spine, bowel and bladder functioning may be affected. In rare instances, nerve compression in this area could lead to cauda equina syndrome (CES), a condition that produces symptoms such as:
• Severe lower back pain
• Numbness, pain, or weakness in one or both legs that may affect the ability to walk or get up from a seated position
• Reduced or altered sensation in the thighs, buttocks, and back of the legs
• Difficulty with urine retention (incontinence)
• Sexual dysfunction that suddenly develops
Symptoms of this nature that may be related to spinal stenosis require emergency treatment. If left untreated, CES may lead to paralysis, bladder infections because of urination issues, or a loss of sensation. If you have any of these symptoms, see a Los Angeles spine surgeon right away.
Symptoms May Spread to Nearby Areas
Even if you’re not experiencing CES or other symptoms suggesting an emergency, spinal stenosis can affect nerves in different ways over time. This sometimes happens as your spine naturally changes with age. For instance, spinal narrowing that only produced occasional pain in the neck, upper back, or lower back may eventually affect nerves that travel to nearby areas. If this happens, you may experience:
• Numbness and weakness that extends to the arms and shoulders—these occur with spinal stenosis in the upper back or neck (cervical spinal stenosis)
• Tingling, pins-and-needles sensations, numbness, or weakness that extends to the thighs, buttocks, or legs if the lower back has a narrow spinal canal
• Shooting or stabbing pain and/or burning sensations in nearby extremities
Quality of Life Can Be Affected
The most compelling reason to be proactive when it comes to treating or managing your spinal stenosis is the impact untreated symptoms could have on your daily quality of life. Because symptoms can range from mild or bothersome to completely debilitating, putting off treatment may affect your ability to:
• Perform work-related tasks
• Go about your daily routine without disruptive pain
• Concentrate on other activities
• Play sports or participate in your favorite activities
• Socialize, if symptoms cause you to avoid certain situations
Surgery is rarely necessary for spinal stenosis. Most people respond well to a combination of conservative treatments. If discomfort is minor, self-care—which might include over-the-counter medications and exercises or stretches you can perform at home—may be recommended. Should symptoms become persistent, opioid painkillers, anti-seizure drugs, or antidepressants may be prescribed. Some patients experience relief from various forms of physical therapy or steroid injections. If these efforts aren’t effective, surgical intervention may be helpful, including coflex back surgery. Los Angeles patients may also have certain structures removed to give nerves more room.
Spinal stenosis can often be managed quite well if it’s diagnosed early. If you suspect you may have spinal stenosis, don’t wait until your pain is severe—see a back specialist as soon as possible. The industry-leading spinal health experts at The Spine Institute are experienced in every aspect of back health and treatment. Call one of our friendly staff today at 310-828-7757 to schedule a consultation.